Files
Download Full Text (1.6 MB)
Publication Date
5-2021
Keywords
oregon; portland; ppmc
Disciplines
Internal Medicine
Description
Introduction Central cord syndrome occurs with a lesion or soft tissue injury affecting the central anatomy of the spinal cord, causing weakness more prominent in the arms than legs, and sensory abnormalities at the level of the lesion. Here I present a case of central cord syndrome caused by a traumatic fall.
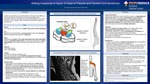
Case Patient A 71 year oldman with history of ESRD, CAD, CHF, and atrial fibrillation HPI Admitted to the hospital after a syncopalevent at home with traumatic falland subsequent development of weakness Exam Weakness was greater in the upper extremities than lower extremitiesand had a left sided predominance. This was accompanied by a severe hyperesthesiaof the upper extremities with severe pain noted on light touch Objective Vital signs: Normal Labs: Unremarkable Imaging CT head: No evidence of bleed or CVA MRI C spine (pictured at right): Multilevel degenerative changes; significant stenosis at C3-C4 with complete effacement of the thecalsac and mild cord compression Clinical Course •Neurosurgery was consulted symptoms attributed to central cord syndrome, not cervical stenosis; invasive intervention was deferred •Syncope was attributed to hypovolemia from persistent vomiting •Weakness slowly improved over the 12 days of hospitalization with physical and occupational therapy •Hospital course was complicated by urinary retention and orthostatic hypotension •Transferred to inpatient rehabilitation for additional 13 days. •At follow up with neurosurgery a few months later, the patient’s weakness had almost completely resolved, no surgical intervention was pursued
Discussion Typical Presentation •Central cord syndrome is most commonly causedby a hyperextension injury of the neckin the setting of preexisting cervical stenosis •Other causes include syringomyeliaor a slow growing tumor •Results in predominantly upper extremity weakness greater than lower extremity weakness, along with sensory abnormalities near the level of the injury, and sometimes bladder dyfunction Pathology •Affects the anterior horn gray matter or the medial aspect of the descending corticospinaltracts, resulting in weakness. •Additionally, disruption of crossing spinothalamicnerve fiberscan result in sensory abnormalities at the level of the lesion. •In our case neurological symptoms resulted from soft tissue swelling and injury after his traumatic fall •Analogous to a concussion of the spinal cord. Management •Central cord syndrome istreated conservatively with an emphasis on physical therapy and supportive management •High dose methylprednisolone can be considered in acute spinal cord injury, but its use is controversial and not currently standard of care •This patient did not receive steroids, and had a good outcome with near complete return of function •Recovery is variable, and can occur over a period of weeks to months
Takeaways • Central cord syndrome causes sensory and motor abnormalities that preferentially affect the upper extremities more than lower extremities due to the arrangement of the neural pathways •Preexisting stenosis of the cervical spinal cord is a risk factor for the development of central cord syndrome, which can occur with a traumatic hyperextension injury •Initial treatment of central cord syndrome is nonsurgical, instead relying on therapy and supportive care while allowing swelling and inflammation to dissipate. Surgical correction of preexisting abnormalities can be considered later in the course, butshould be delayed until initial healing and recovery has occurred, and is not essential to management.
Clinical Institute
Neurosciences (Brain & Spine)
Specialty
Internal Medicine
Specialty
Graduate Medical Education
Conference / Event Name
Academic Achievement Day, 2021
Location
Providence Portland Medical Center
Recommended Citation
Bender, Christopher and Powell, Jesse, "Adding Incapacity to Injury: A Case of Trauma and Central Cord Syndrome" (2021). Providence Portland Medical Center Internal Medicine 2021. 2.
https://digitalcommons.providence.org/oaa_ppmc_21/2