Files
Download Full Text (1.4 MB)
Publication Date
5-2021
Keywords
oregon; portland; ppmc
Disciplines
Internal Medicine
Description
Case Presentation
A 42-year-old female with a past medical history of schizoaffective disorder recently discontinued on multiple psychiatric medications, stable HIV, and hypothyroidism presented with a chief complaint of diffuse extremity weakness and Parkinsonism-like symptoms. History of Present Illness •4-month history of jerking leg movements bilaterally •2-week history of ”feeling paralyzed” with difficulty ambulating •Recent long-term hospitalization at a psychiatric facility as a ward of the state •Multiple changes to psychiatric medication regimen, including abrupt discontinuation of clozapine and risperidone •Abrupt onset confusion at facility and decreased level of interaction at facility prior to admission Exam •T 98.8F, BP 114/66, P 73, RR 18, SpO2 94% on room air •Neck: thyroid without nodules or enlargement •Neuro: CN II-X intact. XI: 0/5 muscle strength on shoulder shrug or head turn. Bilateral shoulder and forearm strength 1/5 bilaterally; hip and thigh flexion/extension 0/5 bilaterally; sensation intact to bilateral upper and lower extremities •Mental status: disoriented to time, place, situation. Oriented to person.
Work Up and Hospital Course
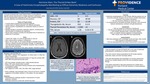
Admission Labs and Work Up: •See Table 1. Calcium 10.8, magnesium 1.6, lithium level 1.2. Other lab values unremarkable •Imaging studies without acute abnormality: CT head w/o contrast, MRI brain, MRI cervical/thoracic/lumbar spine •CSF fluid analysis: elevated protein, mildly elevated glucose •Blood, CSF, urine cultures show no growth •Continuous EEG: generalized slowing consistent with encephalopathy; no epileptiform activity •CSF negative for VDRL, HSV, VZV, EBV, CMV, fungal elements •Ativan challenge: 2mg lorazepam every 2 hours for 24 hours; if positive, suggestive of neuroleptic catatonia. In this patient, this was negative Treatment: •Dexamethasone challenge resulted in improvement of muscle weakness, confusion •Prolonged prednisone course with months-long taper
Discussion
Overview •Hashimoto encephalopathy is a rare disorder affecting patients who are commonly euthyroid, thought to be an immune complex inflammatory response in the cerebral vasculature •HE more commonly affected by women than men •It is characterized by fluctuating neurologic symptoms, most commonly behavior disturbances, confusion, and gait disturbances DIAGNOSIS •TSH can range from euthyroid to hypothyroid •TPO Ab and thyroglobulin Ab are commonly significantly elevated •CSF findings: elevated protein, lymphocytic infiltrate •EEG: non-specific slowing suggestive of encephalopathy •MRI: normal, some cases with focal hyperintensity MANAGEMENT •High dose prednisone with a prolonged course and taper; often months •>90% respond to corticosteroid therapy •IVIG and plasmapheresis have shown improvement in some cases
Conclusion
• Here we present a 42-year-old female with a rare case of Hashimoto encephalopathy manifesting as confusion and weakness •The most common clinical presentations for HE include cognitive impairment, ataxia, and focal neurologic deficits •This case demonstrates that presentation of a primary autoimmune disorder can manifest despite normal TSH and unrevealing imaging findings •This patient responded to high dose prednisone for 2 weeks with a prolonged taper and 4 days of IVIG with resolution of muscle weakness and confusion
Specialty
Internal Medicine
Specialty
Graduate Medical Education
Conference / Event Name
Academic Achievement Day, 2021
Location
Providence Portland Medical Center
Recommended Citation
Paiva, Cody and Clark, Brinton, "Hormone Wars: The Thyroid Strikes Back! A Case of Hashimoto Encephalopathy Manifesting as Diffuse Extremity Weakness and Confusion" (2021). Providence Portland Medical Center Internal Medicine 2021. 7.
https://digitalcommons.providence.org/oaa_ppmc_21/7