Files
Download Full Text (648 KB)
Publication Date
4-29-2020
Disciplines
Internal Medicine
Abstract
INTRODUCTION: Lemierre’ssyndrome is a rare and potentially fatal complication of acute pharyngitis most commonly seen in healthy, young adults who present with neck pain and persistent, high-grade fever. It is caused by anaerobic gram-negative organisms, most often Fusobacteriumnecrophorum, spreading into the deep spaces of the neck. This leads to septic thrombophlebitis of the internal jugular vein (IJ) with septic emboli, most frequently to the lungs.
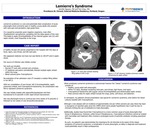
CASE REPORT: A healthy 18-year-old woman presented to the hospital with five days of fever, rigors, sore throat, and left neck pain. She appeared relatively non-toxic but was febrile to 105.6℉ and in septic shock. Her source of infection was initially unclear. Her work up included: • Normal CT neck with contrast and urinalysis. • CT abdomen and pelvis coincidentally showed multiple septic emboli within the lungs. • Blood cultures grew F.necrophorum. Re-evaluation of her admission neck CT revealed a modest filling defect in her left IJ. With her constellation of sore throat, left IJ thrombophlebitis, septic pulmonary emboli, and F.necrophorumbacteremia, her presentation was felt to represent Lemierre’ssyndrome. She was initially treated with piperacillin/tazobactamand then transitioned to IV penicillin G with rapid clinical improvement. She was discharged home to continue two more weeks of IV penicillin G followed by two weeks of oral amoxicillin/clavulanate.
DISCUSSION: What constitutes Lemierre’ssyndrome is controversial however the “classic” Lemierre’ssyndrome case consists of: • Healthy, young adult with pharyngitis. • Within 4-5 days, develops worsening neck pain, sore throat, high fevers, and rigors. • F.necrophorumbacteremia with jugular venous thrombophlebitis and disseminated septic emboli. • Most common sites for septic emboli include the lungs, joints, soft tissue, and abdomen. In retrospect, my patient’s clinical presentation was typical for Lemierre’ssyndrome, even before her blood cultures resulted with F.necrophorum. Although a rare disease with an incidence of approximately one per million persons per year, there has been a resurgence of reported cases since the 1990’s which some people hypothesize may in part be due to clinicians limiting the use of antibiotics to treat pharyngitis. Additionally, studies have found that F.necrophorumis a more common cause of acute pharyngitis than Group A Streptococcus. However, unlike Group A Streptococcus, F.necrophoruminfections cannot be treated with macrolides and treatment often involves a prolonged course of penicillin antibiotic including parenteral therapy. As such, my patient’s case demonstrates the importance for all internists to be aware of the classic symptoms of Lemierre’ssyndrome, a complication of acute pharyngitis, as delay in diagnosis and treatment could potentially result in fatal consequences.
Specialty/Research Institute
Internal Medicine
Specialty/Research Institute
Graduate Medical Education
Conference / Event Name
Academic Achievement Day, 2020
Location
Providence St. Vincent, Internal Medicine Residency, Portland, Oregon