Files
Download Full Text (3.6 MB)
Publication Date
4-29-2020
Disciplines
Internal Medicine
Abstract
Background: In persons who presents with fever, rectal pain and bleeding, CMV proctitis should be considered if other workup is negative, especially if recent unprotected anal receptive intercourse.
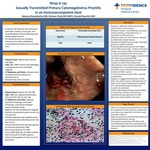
Case Presentation: A 26-year-old bisexual man presented with chief complaints of fever, malaise, rectal pain, and rectal bleeding after anal insertion of foreign body. He initially denied any unprotected sexual intercourse. CBC, CMP, stool pathogen, rectal gonorrhea, and rectal chlamydia were unremarkable. He returned after 1 week with the similar complaints, however admitted to unprotected anal receptive intercourse a month prior. His vitals were notable for temperature of 102 with tachycardia to 108. Labs were significant for WBC 6.6, atypical lymphocytes 22%, ALP 173, AST 72, and ALT 146. CT AP with contrast showed perirectal fat stranding, rectal wall thickening, and several perirectal lymph nodes. Syphilis and HIV testing were negative. Given concern for viral proctitis from HSV, he was treated with valacyclovir. Flexible sigmoidoscopy showed diffuse severe inflammation with deep ulcerations consistent with severe ulcerative proctitis extending 15cm into the rectum. Biopsies were positive for CMV on immunohistochemical staining and viral culture. CMV serology was positive for IgM, IgG, and viral DNA. The patient was treated with ganciclovir for primary CMV proctitis for a 14-day course.
Conclusion: Proctitis typically presents with rectal bleeding, rectal pain, anorectal itching, cramps/tenesmus, or discharge from the anal canal. Common sexually transmitted infectious causes include chlamydia, gonorrhea, syphilis, HSV. CMV has also been shown to be a cause of procto-colitis in immunocompromised patients with HIV. Though rare, primary CMV in an immunocompetent host can cause proctitis and has been reported in persons who engage in unprotected anal intercourse, especially MSM. Diagnosis of primary CMV proctitis requires multiple diagnostic tests in the right clinical setting. Detection of CMV IgM, a four-fold increase in CMV IgG done 2-4 weeks apart, and sigmoidoscopy showing rectal mucositis or ulceration are suggestive of CMV proctitis. In our patient, his atypical lymphocytes and elevated liver function tests were also suggestive of CMV. Biopsy showing presence of inclusion bodies or basophilic intranuclear inclusions and immunohistochemical staining that is positive for CMV are confirmatory. Treatment for primary CMV proctitis has not been well defined and is typically conservative management though we chose to treat with ganciclovir given severity of symptoms. In conclusion, a mononucleosis-like illness with rectal bleeding and/or pain after unprotected anal intercourse can suggest a diagnosis of CMV proctitis.
Specialty/Research Institute
Internal Medicine
Specialty/Research Institute
Graduate Medical Education
Conference / Event Name
Academic Achievement Day, 2020
Location
Providence Portland Medical Center, Internal Medicine Residency, Portland, Oregon